Pulmonary hypertension: A simple guide
Pulmonary hypertension (PH) damages the right side of the heart, creating problems delivering oxygen-rich blood throughout the body. Without treatment, PH results in heart failure. But early detection of PH allows for early treatment and improved outcomes.
What is pulmonary hypertension? #
Pulmonary hypertension means that you have high blood pressure in your pulmonary arteries, the vessels that carry deoxygenated blood from the heart to the lungs.
Many people mistake PH for “regular” hypertension, but they’re two different conditions. Hypertension, also called high blood pressure or systemic hypertension, means that pressure in the arteries is higher than it should be throughout the entire body. In this case, you can monitor high blood pressure with a blood pressure cuff.
Pulmonary hypertension, on the other hand, explicitly affects the vessels within the lungs and the pulmonary arteries. With PH, vessels become damaged and narrow, losing elasticity. When this damage occurs, the right side of the heart works much harder to pump blood through.
People in the initial stages of PH often experience symptoms that also present with other common medical conditions. They feel short of breath and tired, have right-sided abdominal pain, and experience a decreased appetite. These common symptoms often delay diagnosis until symptoms escalate to ankle swelling, chest pain, dizziness, and heart palpitations.
Failing to treat PH can eventually lead to heart failure.
How common is pulmonary hypertension? #
It’s unknown how many people have PH. However, estimates show that 50 to 70 million people worldwide live with it. PH commonly affects older adults, although adults of any age can get it. Worldwide, about one out of every ten people over the age of 65 lives with PH. According to researchers, this number will likely rise within the next few decades.
People with certain lung and heart conditions, like mitral or aortic valve diseases, scleroderma, sickle cell, and HIV, face a greater risk for PH.
What causes pulmonary hypertension? #
PH often occurs from underlying medical conditions, diseases, and exposures to environmental toxins. High blood pressure in the lungs’ arteries can occur from some congenital heart diseases, coronary artery disease (CAD), liver cirrhosis, blood clots in the lungs, and connective tissue disease.
Lung problems are another common cause of PH. COPD, including chronic bronchitis and emphysema, interstitial lung disease, and obstructive sleep apnea (OSA), can also lead to PH.
How is pulmonary hypertension diagnosed? #
Physicians diagnose pulmonary hypertension with a series of tests.
- Electrocardiogram (EKG or ECG)
- Heart catheterization
- Six-minute walk test
- Assessment
Once your physician diagnoses PH, the next step is determining the cause.
- Computerized tomography, also called CT or CAT scans, checks for lung diseases or blood clots in the lungs.
- Sleep studies rule out sleep apnea, which causes you to stop breathing during sleep temporarily.
- Lab testing helps rule out other specific medical conditions.
- Pulmonary function testing (PFT) determines if you have obstructive lung disease.
The physician diagnoses secondary pulmonary hypertension if these tests determine a cause of PH. If there’s no known cause, it’s known as primary pulmonary hypertension.
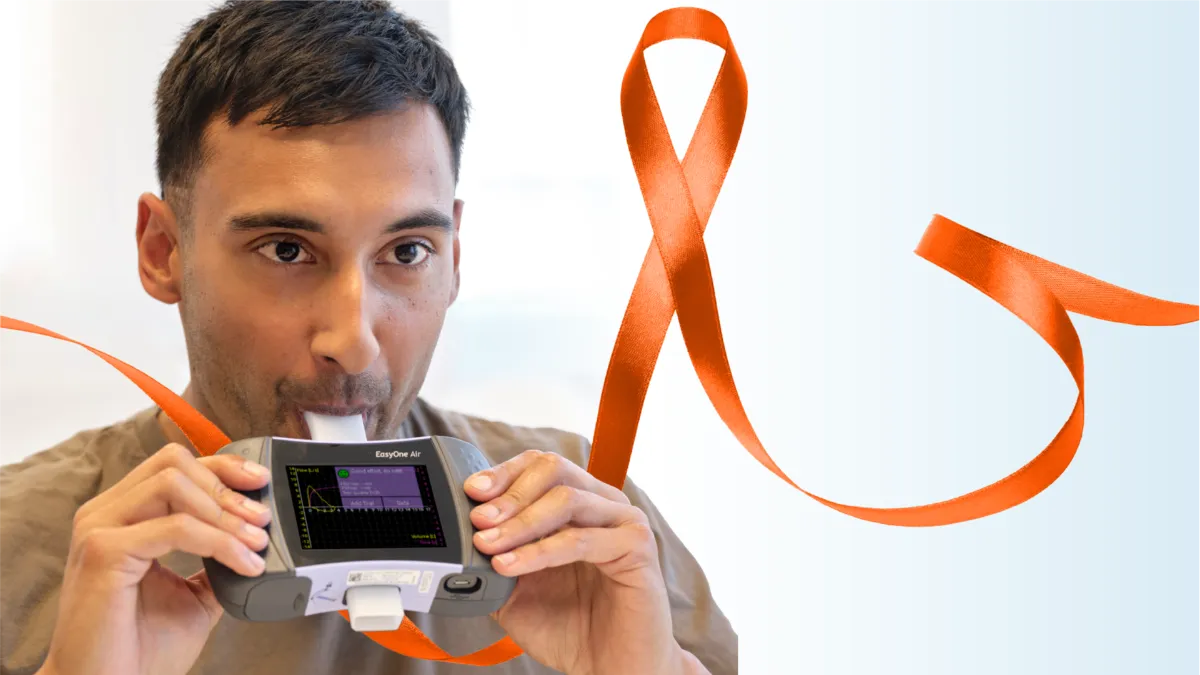
Pulmonary function testing for pulmonary hypertension #
PFTs measure how air moves in and out of the lungs, how much air the lungs can hold, and how well gas exchange occurs. Many people with PH have lung disease, like COPD or pulmonary fibrosis, and may require a treatment plan.
PFT measurements including FVC/DLCO and FVC/DLCO/VA can provide a non-invasive way of detecting early signs of PH. Research shows that early diagnosis of PH improves its outcome. Obtaining an early diagnosis allows the healthcare team to establish an early treatment plan that slows down, prevents, and possibly even reverses severe consequences of the disease.
A follow up appointment with a specialist may be recommended to confirm diagnosis.
Clinical statements come from these sources:
https://medlineplus.gov/pulmonaryhypertension.html
https://phassociation.org/patients/aboutph
https://my.clevelandclinic.org/health/diseases/6530-pulmonary-hypertension-ph
https://www.lung.org/lung-health-diseases/lung-procedures-and-tests/six-minute-walk-test
https://www.ucsfhealth.org/en/conditions/pulmonary-hypertension/diagnosis
https://www.europeanreview.org/wp/wp-content/uploads/6658-6664.pdf