Long COVID: What are the long-term effects?
With as many as 40% of people experiencing symptoms 100 days after their COVID diagnosis, what impact will COVID have on the respiratory health of recovering patients?
Long COVID, or post-COVID syndrome #
Each day of the COVID-19 pandemic has brought another surprise, another mystery, another learning opportunity. In the early days, challenges were mostly comprised of figuring out how the SARS-CoV-2 virus spreads, therapeutic options, and the like. Working to prevent the spread of the virus was a top priority, even as the work toward a vaccine ramped into high gear. New symptoms were considered, additional related syndromes were evaluated, and progress was made toward figuring out how to get people not only out of the hospital, but to stop them from going in the first place.
Questions remain, but those that have been answered have created an entirely new question set for researchers and clinicians: what are the long-term effects of COVID-19 for those who recover? Most people appear to recover fully from COVID-19 and return to their baseline health. However, in the late spring and early summer of 2020, a strange phenomenon began to appear: A significant number of people who made it through acute COVID-19 illness continued to experience symptoms weeks, even months after their ‘recovery.’ Thus, the term Long COVID, or post-COVID syndrome was coined.
What do we know about post-COVID syndrome? #
Even more curious, this Long COVID seemed to strike with little rhyme or reason. The usual risk factors for disease sequelae, like hospital admission, intubation, etc., seemed to have little bearing on whether someone became a so-called ‘long-hauler.’ Otherwise, young, healthy individuals were finding no end to their fatigue, respiratory complications, and other effects.
Trying to ascertain what the respiratory repercussions of Long COVID-19 will be, an Austrian team developed a prospective multi-center study to gauge at least the medium-term effects. Recently published in the European Respiratory Journal as Cardiopulmonary recovery after COVID-19 – an observational prospective multi-center trial,” the team’s output offers some compelling context into post-acute recovery, but also perhaps some hope for the future1.
It’s most common these days to refer to the SARS-CoV-2 pathogen as ‘the coronavirus,’ probably because it’s the one grabbing the most attention. However, it’s important to remember that this bug is merely the latest in a series of coronaviruses. This type of virus has been known to science since the 1960s (and most likely known to humanity for far longer) and has wreaked havoc on our societies before.2 Looking at some of those previous outbreaks (specifically the 2012 Middle Eastern outbreak of the MERS-CoV virus and the infamous 2002 SARS episode), the Austrian team found multiple studies demonstrating the development of fibrotic tissue within the lungs of roughly a third of survivors.
Long term effects of COVID-19 on respiratory health #
Considering the current virus shares a great deal of genetic similarity with both of these pathogens (particularly its namesake, now called SARS-CoV-1), researchers have feared an explosion of pulmonary fibrosis cases that could strain the public health and ambulatory care systems as severely as the acute illness has overwhelmed the acute care setting. This study was therefore set up to focus on fibrotic indicators, including general dyspnea scores (specifically the modified Medical Research Council (mMRC) score), pulmonary function testing (including diffusion/transfer capacity), and low-dose thoracic CT scans. Some additional testing (such as echocardiography) was also done, owing to the interplay between the respiratory and vascular systems, particularly when it comes to the strain of fibrosis. Patients were included after a PCR-confirmed diagnosis of COVID-19 and were asked to follow up twice, once at 60 days and once at 100 days.
How common is Long COVID? #
The findings were striking from a clinical perspective. Approximately one-quarter of the cohort reported some degree of sleep disruption (including night sweats and newly-diagnosed sleep disorders), and nearly 40% reported ongoing issues with dyspnea at the 100-day follow-up visit. Imaging data presented similarly bad news, with 63% of subjects demonstrating abnormalities including ground-glass opacities and ongoing consolidation, generally focused on the lower lobes of both lungs. Pulmonary function testing was not much better, with a third of the subjects demonstrating defects in their DLCO measurementsor lung volumes at the second visit. Most of the group also showed signs of hypoxemia, with a solid 20% of them having a pO2 of 65 mmHg or lower at rest.
Again, to put these numbers into context, the second follow up occurred a full three months after these patients were declared ‘out of the woods.’ It is also important to note that while post-acute sequelae are not uncommon in a variety of critical illnesses (ARDS, for example), only 22% of these patients were admitted to the ICU during their hospital stay.
That means even relatively mild cases of COVID-19 have the potential to have major effects on lung function and quality of life that linger well past discharge and likely impact medical, social, and other aspects of recovery. One hundred days may not sound like a particularly long time, but it’s certainly long enough to have major socioeconomic disruptions, such as the loss of a job and attendant economic issues, as well as the potential development of anxiety, depression, post-traumatic stress associated (frequently noted in ARDS survivors), and other mental health concerns.
Is Long COVID permanent? #
Fortunately, the data are not completely disheartening. Significant improvements were noted between the first follow-up visit and the second in virtually every category, including functional status, lung functions, and most of the radiographic anomalies. As the authors mention, this lines up well with previous studies covering things like the aforementioned ARDS (as well as the original SARS itself), with most functions returning to physiological normal within a year of the insult.3
In addition, the authors are careful to note that as this study began in the early phases of the pandemic, it was somewhat difficult to acquire pre-COVID-19 cardiopulmonary evaluations on many of their patients, leaving open the possibility that a certain percent had underlying problems that were simply illuminated by their COVID-19 experience. Certain technical limitations introduce some uncertainty as well, such as the difficulty in teasing out early-stage fibrosis development from late-stage inflammation on the verge of resolving.
Taken together, these limitations do provide some reason for optimism. While the risk of serious sequelae certainly exists, there is not yet compelling evidence that a massive epidemic of pulmonary fibrosis or similar condition is on the horizon. There is certainly reason to hope that most COVID-19 survivors will return to their pre-COVID breathing status and not require ongoing rehabilitation programs or other therapies. And the lessons that continue to be learned about the acute treatment of COVID-19 will minimize the risk of ancillary insults (such as ventilator-associated lung injuries) that can also cause permanent damage.
How can we mitigate the effects of Long COVID? #
There are still a tremendous number of unknowns when it comes to COVID-19. We still don’t know ultimately how effective the approved (and upcoming) vaccines will be in tempering the pandemic. We don’t know how long phrases like ‘social distancing’ and ‘mask up’ will be a part of our vocabulary. And we don’t entirely know what the future will look like for COVID-19 survivors and their caregivers.
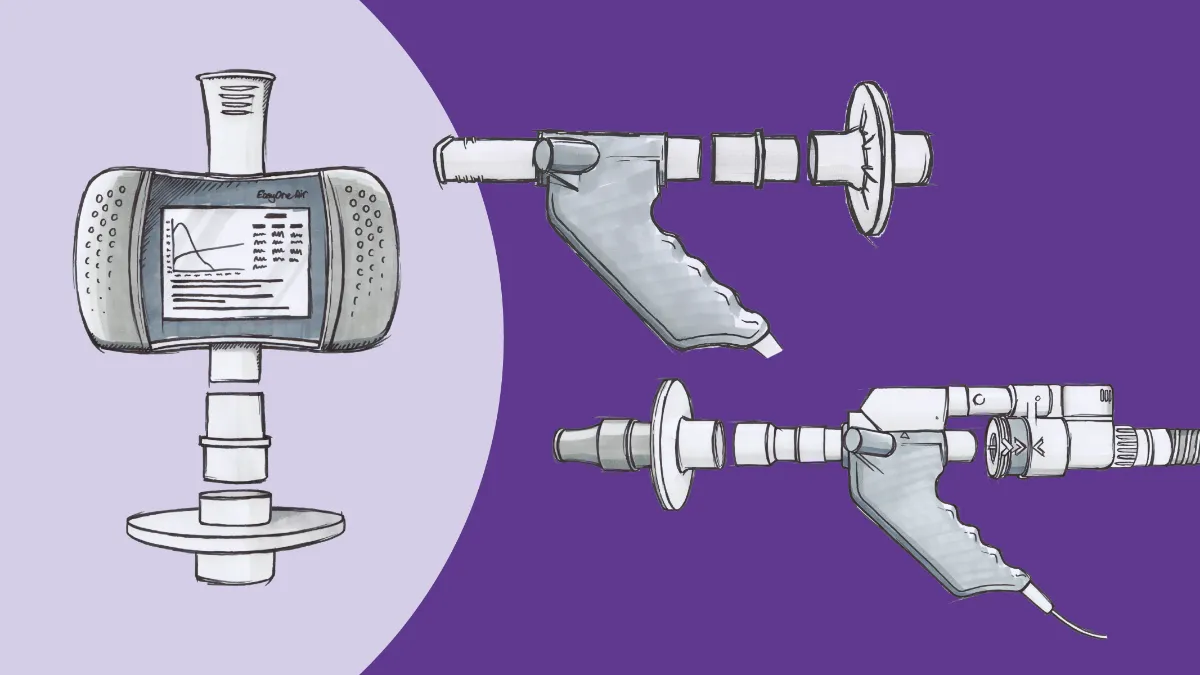
However, those unknowns also represent a tremendous number of opportunities and responsibilities for clinicians. As we continue to move forward into new phases of the pandemic, pulmonary function testing will play a critical role in determining the length and severity of respiratory-related sequelae, and the public health system will be heavily reliant upon the PFT community for answers. The preliminary indications are that Long COVID will be a largely restrictive process that interferes with gas transfer, so office-based basic spirometry may not be enough to provide all those answers.
As rehabilitation and recovery programs for COVID-19 long-haulers become better defined, the PFT community will play a large role in working with these programs to define eligibility and efficacy standards. It’s abundantly clear that DLCO testing in post-COVID patients is key to the long-term care of their pulmonary health.
These studies represent the first steps forward in identifying the risk factors and physiological changes involved after the resolution of ‘acute’ COVID-19. They were small studies, owing to the complexities and timeframes involved in such studies, but they provide important insights into what the disease potentially does to people, particularly to their lungs. It is an important starting point that gives the clinical community a foundation to build subsequent studies and improve understanding of what to look for in COVID-19 survivors to more effectively treat the sequelae. It also represents both hope and opportunity for the PFT community and demonstrates the important role this specialty will play in the public and community health space in the years to come.
Sonnweber T, Sahanic S, Pizzini A, et al. Cardiopulmonary recovery after COVID-19 - an observational prospective multi-center trial. Eur Respir J. December 2020. doi:10.1183/13993003.03481-2020 ↩︎
Kahn JS, McIntosh K. History and Recent Advances in Coronavirus Discovery. Pediatr Infect Dis J. 2005;24(Supplement):S223-S227. doi:10.1097/01.inf.0000188166.17324.60 ↩︎
Bein T, Weber-Carstens S, Apfelbacher C. Long-term outcome after the acute respiratory distress syndrome: Different from general critical illness? Curr Opin Crit Care. 2018;24(1):35-40. doi:10.1097/MCC.0000000000000476 Zhang P, Li J, Liu H, et al. Long-term bone and lung consequences associated with hospital-acquired severe acute respiratory syndrome: a 15-year follow-up from a prospective cohort study. Bone Res. 2020;8(1). doi:10.1038/s41413-020-0084-5 ↩︎