The history of PFT - part 2
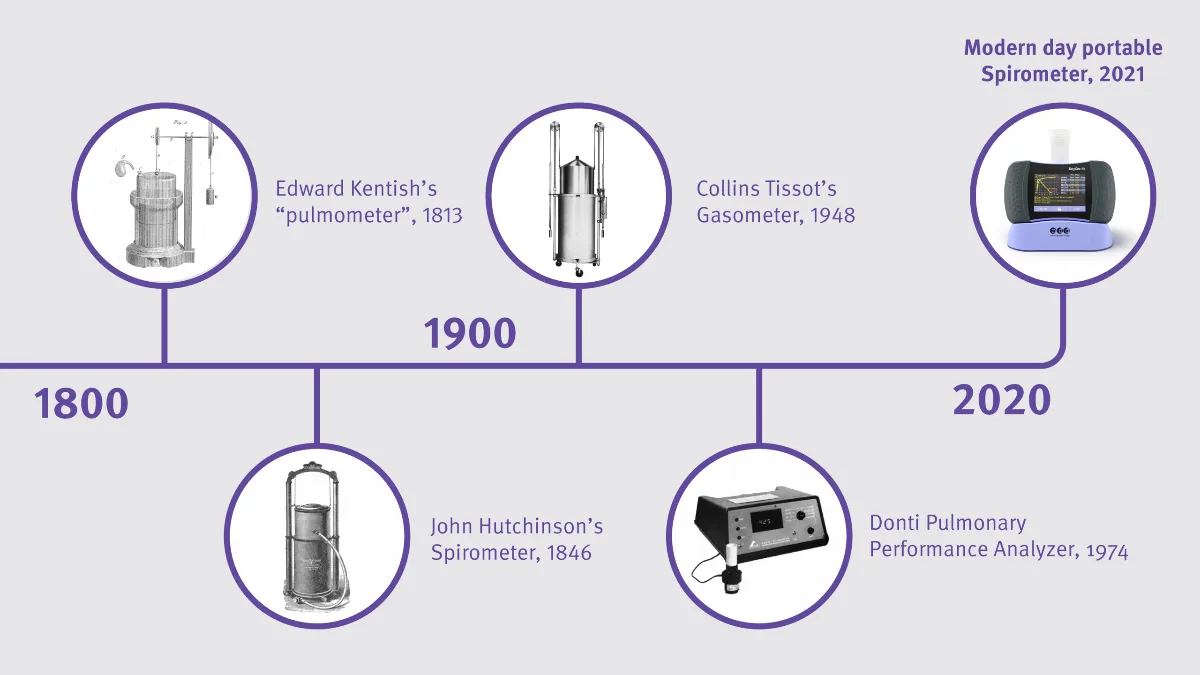
It’s easy to take pulmonary function testing for granted these days. After all, technology has literally put spirometry in the palm of your hand, and even equipment for more complex testing like diffusion capacity can now be made easily portable. But in order to really understand how remarkable these accomplishments are, it’s important to understand where it all began. This is Part 2 of our ongoing series on the history of pulmonary function testing.
Read from the start - The history of PFT - Part 1.
Using spirometry to capture data #
With a decade or so of vital capacity data (collected by the redoubtable John Hutchinson in our last episode), it would be easy for one to assume that a golden age of pulmonary function testing was about to begin. It would also be easy for one to be wrong.
Even with that plethora of data, spirometry remained essentially a novelty, at least in the clinical realm. This was, after all, still an era of relative medical naiveté, transitioning from the idea of illness being caused by an imbalance of bodily humours and into modern medical theories. Florence Nightingale was still merely on the cusp of opening her nursing school, and Johns Hopkins Hospital was still decades away from opening and establishing now-common practices like residencies for new physicians. Much of our current practice was still on the horizon, and while the spirometer was an interesting new tool, it was still too unknown for many of the day’s clinicians to utilize on a regular basis.1
Nevertheless, there was still significant interest in figuring out if not by humours and miasmas, then how exactly did all the internal workings of the human body perform together? So, while the clinical applications remained limited, boundless research opportunities presented themselves (particularly in the nascent field of biostatistics), and the spirometer was a more-than-capable tool to measure chest and lung functions.
The importance of mass pulmonary function testing #
Many of the first mass research and data collection projects came from the world’s militaries. With large pools of subjects with varying anthropometric characteristics close at hand (considering both then-current and prospective soldiers), it was relatively easy to collect large-scale data in a short amount of time.
Tasked with one of the first known large-scale studies of Army men was no less a figure than Fredrick Law Olmsted, perhaps best known as one of the architectural minds behind New York City’s Central Park.2 As the American Civil War flared in 1861, Olmsted left his post as park superintendent to serve as Executive Secretary of the U.S. Sanitary Commission, an agency dedicated to caring for wounded Union soldiers3. In this role, Olmsted saw an opportunity to better understand the makeup of the volunteer force (having undertaken a similar effort analyzing the labor workforce building Central Park).
Challenges in early pulmonary function testing #
Olmsted left the Sanitary Commission in 1863, having collected data (including spirometry) on some 8,000 soldiers. The work was then picked up by another non-clinical scientist by the name of Benjamin Gould. An astronomer by training (in fact, the first person in the United States to earn a doctorate in astronomy), Gould was nevertheless one of the founders of the National Academy of Sciences and, therefore, well-versed in the scientific methods needed to complete a study of this scale.4
As a proponent of John Hutchinson, Gould set out to expand upon (and correct where necessary) Hutchinson’s spirometric tables with a tremendous cohort of over 21,000 soldiers (as well as some prisoners). Notably, this study also included (for perhaps the first time) a sizable contingent of African American subjects, as these soldiers had recently begun to see significant duty.
Capturing reliable results in early pulmonary function testing #
There was, however, significant pressure to get the data quickly to make better predictions about potential recruits. Today, that pressure, combined with the other difficulties inherent in conducting human research during wartime (occasionally even quite close to actual combat), would likely raise questions about data integrity and collection methods. Indeed, some questions were raised by one of the project’s chief data analysts, Lucius Brown.
In a May 1869 letter to Gould, Brown warned against lost data, miscategorized data, and overall concerns about accuracy. One of Brown’s greatest concerns was regarding the intermingling of ethnic data, with subjects of mixed race being included in with various other categories. In the overall data, this led to supposedly distinct differences in lung function between the races, therefore confirming many pre-existing beliefs about those of African descent. In truth, Lucius Brown pointed out in his letter that, “The personal equation is evidently very large so that it is not possible to compare the white and the colored races with any certainty of being right.2”
However, Benjamin Gould’s stature as a scientist overrode many of those questions, especially since he was more than willing to consult with those more experienced in physiology. Brown continued to assist with the analysis, with some of the details of his concerns and possible data corrections lost to history. Summarized tables of findings, grouped by the subjects’ presumed ethnicity, occupation, and whether or not they were “in normal vigor” were then assembled and published as part of a tome entitled Investigations in the Military and Anthropological Statistics of American Soldiers5.5
Does ethnicity contribute to pulmonary function? #
As these data reinforced beliefs common to the time, they went essentially unchallenged at the time of publication. What is now known as social determinants of health were still largely hypothetical, and other potential confounding factors such as age and relative health (other than the vague “usual vigor”) went unaccounted for.
However, not long after Gould’s investigations was published, another military epidemiological study was undertaken, this time headed by the Chief Medical Officer of the Bureau of the War Department, Colonel Jedediah Baxter. Having served as regimental and brigade surgeon in various locations throughout the Civil War, Baxter had far more hands-on clinical experience than Benjamin Gould, which likely led him to approach anthropometrics from a far different perspective, which in turn led to markedly different conclusions.
Under Baxter’s watch, the Army completed a study that was larger (with over a million subjects) and simpler than Gould’s effort. 6Lung health was still considered an important enough component of vitality to be evaluated in this work, but rather than relying upon the still relatively new technology of the spirometer. Baxter opted to use predicted values and calculations derived from efforts like Hutchinson’s and Gould’s, not entirely dissimilar to a clinician today using NHANES III or GLI tables.
By measuring chest circumference at maximal inhalation and maximal exhalation, Baxter and his team were able to extrapolate each soldier’s vital capacity with a reasonable enough (for the time) degree of accuracy. In contrast to Gould, Baxter found no significant difference in these measurements based on ethnicity; in fact, the colonel was just as intrigued by the differences in the men of various European descents as he was by those of the freedmen.
Why standardization is important in pulmonary function testing #
Why these two scientists examined similar data and arrived at wildly different conclusions is not clear. It is certainly possible their conclusions were swayed by their relative experiences; Gould studied hard numbers in the context of prevailing biases, while Baxter’s history as a clinician helped him identify the humanity behind those numbers. The data harvesting techniques were clearly different, potentially introducing some error; while anthropometrics is used to make predicted values today, certainly not every patient lines up with those predictions. Certainly, the troubled racial politics of the day had some impact, with Baxter explicitly calling out the idea that a label like ‘Colored’ was imprecise and nonscientific and Gould aligning with prevailing views on racial superiority and inferiority.
Gould’s legacy #
In any event, Gould’s assertions (likely due to having been published first) influenced a variety of subsequent anthropologists, including no less a mind that Darwin himself, who references Gould’s data and theories throughout his later theories on the origin of the human species.7 Indeed, correction for ethnicity can still be found throughout modern-day pulmonary function devices alongside height, age, and biological sex designators.
The debate over whether these corrections should still be in use also persists, particularly since hospitals and healthcare systems have been re-evaluating implicit biases throughout 2020.8 Surely, any answers will be complex; much like a chest X-ray, lung issues must be interpreted in shades of gray, not simply black or white.
Reiser S. Medicine and the Reign of Technology -. Cambridge University Press; 1981. ↩︎
BRAUN L. Spirometry, Measurement, and Race in the Nineteenth Century. J Hist Med Allied Sci. 2005;60(2):135-169. http://www.jstor.org/stable/24632252. ↩︎
Stille C. History of the United States Sanitary Commission Being the General Report of Its Work during the War of the Rebellion.; 1866. https://archive.org/details/historyofuniteds00stiluoft. Accessed December 15, 2020. ↩︎
Benjamin Gould. http://www.nasonline.org/member-directory/deceased-members/20001444.html. Accessed December 15, 2020. ↩︎
Gould B. Investigations in the Military and Anthropological Statistics of American Soldiers. https://books.google.com/books?id=FTYAAAAAQAAJ&printsec=frontcover&source=gbs_ge_summary_r&cad=0#v=onepage&q&f=false. Accessed December 17, 2020. ↩︎ ↩︎
Baxter JH. Statistics, Medical and Anthropological, of the Provost-Marshal-General’s Bureau, Derived from Records of the Examination for Military Service in the Armies of the United States during the Late War of the Rebellion … Comp. … by J.H. Baxter … Washington : Govt. Print. Off.,; 1875. doi:10.5962/bhl.title.24900 ↩︎
Darwin C. The Descent of Man.; 1871. https://www.penguinrandomhouse.com/books/300275/the-descent-of-man-by-charles-darwin/. Accessed December 18, 2020. ↩︎
Braun L. Race Correction and Spirometry. Chest. 2020;0(0). doi:10.1016/j.chest.2020.10.046 ↩︎