The truth about COPD
According to the Global Burden of Disease Study in 2016, 251 million people were living with Chronic Obstructive Pulmonary Disease (COPD), with many undiagnosed cases.
The primary source for all statements can be found here:
https://www.who.int/news-room/fact-sheets/detail/chronic-obstructive-pulmonary-disease-(copd)
According to the Global Burden of Disease Study in 2016, 251 million people lived with Chronic Obstructive Pulmonary Disease (COPD). COPD is a progressive and life-threatening lung disease that causes shortness of breath, predisposes exacerbations (or flair-ups) and serious illness.
It’s an umbrella term that encompasses multiple, independent lung diseases including Emphysema and Chronic Bronchitis. While there have been significant improvements in the education, awareness, and mitigation efforts, unfortunately, COPD has quickly risen to the third-leading cause of death in the United States of America in recent years.
Although research continues to discover better methods of treating this non-curable lung disease, diagnosis; specifically, the accurate diagnosis of COPD is a crucial first step in helping a patient live with it.
In the information below, we’ll provide a roadmap that will explore several of the facts about COPD. We’ll explain several of the symptoms, risk factors, who are at higher risk, how the disease is diagnosed, and some of the treatments and resources available to patients, their caregivers, and medical professionals.
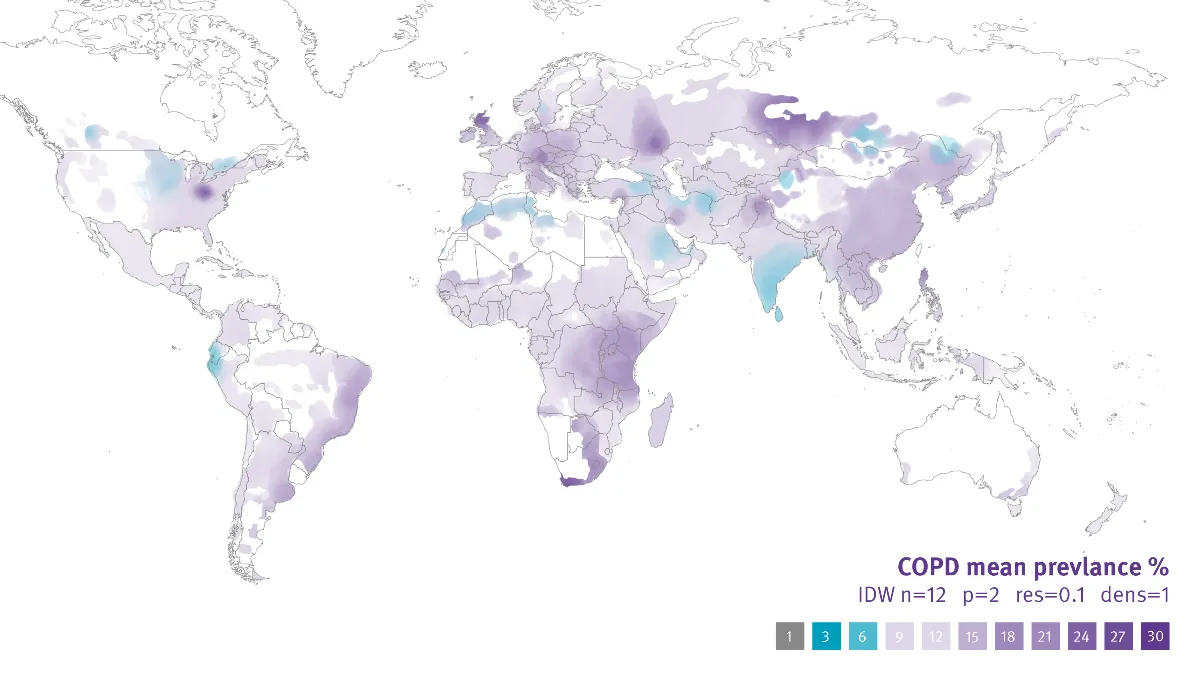
The prevalence of COPD worldwide #
Chronic Obstructive Pulmonary Disease has become a global epidemic in recent years. Globally, it was estimated in 2015 that 3.17 million deaths were caused by the disease, which represented five percent of all fatalities. However, 90 percent of these deaths occur in low and middle-income countries.
Whether this is due to reduced medical resources, exposure to common risk factors, or social choices, the simple truth is that several COPD cases can be prevented. Before we explore the risk, factors and introduce proactive ways of reducing the potential of developing COPD, let’s outline some of the numbers.
COPD statistics #
COPD happens to be the third leading cause of death and ranks ninth for lost disability-adjusted life years, resulting in considerable global morbidity and mortality1. However, the disease itself is not always the cause of death. In many cases, it’s a comorbidity factor such as ischemic heart disease and cerebrovascular disease that ultimately leads to the patient fatality.
The lack of physical activity can likewise lead to secondary disease diagnoses such as Type II Diabetes, kidney failure, and cardiovascular disease. A study investigating factors associated with new-onset diabetes in the UK concluded that patients with frequent exacerbations of COPD and cardiac comorbidities, such as hypertension and heart disease, were more likely to develop type 2 diabetes mellitus (T2DM).
Some of the common treatments such as inhaled corticosteroid (ICS) can also increase the incidence of COPD.
COPD diagnosis statistics #
While the numbers above are shocking, arguably the most alarming statistic is that as many as 50 to 90% of COPD cases remain undiagnosed or improperly diagnosed.2 Under-recognition of respiratory symptoms happens to be the prime reason for the misdiagnosis of the disease. However, the use of inaccurate or outdated spirometry and pulmonary function testing (PFT) devices also represents a hurdle to medical professionals.
What are the risk factors for COPD? #
As most of us know, the lungs and the efficient inhalation of oxygen and corresponding exhalation of carbon dioxide are crucial to the overall health of organs such as the heart, kidneys, liver, and brain. The more-efficient and healthy our lungs operate – the easier it is for our bodies to process energy-producing oxygen.
COPD is an obstruction in the respiratory system which reduces the lungs’ ability to inhale and exhale. This obstruction occurs when toxins, chemicals, pollution, or previous respiratory infections cause progressive damage to different parts of the lungs. Certain blood conditions or hereditary factors such as Alpha-One can accelerate the development of COPD.
Without question, the primary cause of COPD is tobacco smoke (including secondhand). Other risk factors may include:
- Poor indoor air quality
- Outdoor air pollution
- Occupational chemicals and dusts (vapors, irritants, and fumes)
- Frequent lower respiratory infections in childhood
- Hereditary factors or in-utero development due to exposure to risk factors by the mother
Who is at risk for developing COPD? #
In years past, COPD was most common in men who were smokers. This created a negative stigma that it was a disease that was ‘self-induced’ due to social choice. However, because of comparably high levels of tobacco smoking among women in high-income countries, and the higher risk of exposure to indoor air pollution (such as solid fuel used for cooking and heating) for women in low-income countries, the disease now affects men and women almost equally.
Smoking is not the only risk factor for COPD. As noted above, those who are frequently exposed to poor air quality in the workplace or at home are also prone to developing COPD. Some of the more common industries that have shown risk factors include:
- Automotive repair
- Manufacturing
- Coal mining
- Fossil fuel exploration and refining
- Casino workers
- Cosmetics and those exposed to indoor irritants
- HVAC, plumbers, pipe-fitters and commercial warehouse workers
Due to these facts, many corporations and industries have enacted occupational health programs that are focused on improving workplace ventilation, air quality, and even completing on-site lung health screening to monitor the performance of employee lung function.
What are the main symptoms of COPD? #
Chuck Morrison, one of the co-founders of Right2Breathe® - a respiratory patient and caregiver-centric non-profit based in New Jersey, was fond of describing COPD as the following, “Imagine breathing through your mouth only. Now imaging closing your mouth and inserting a straw to breathe through. Finally, climb a set of stairs with that straw as your only source of oxygen and exhaling carbon dioxide.”
As the name implies, COPD is an obstruction in the lungs and reduces the patient’s ability to breathe. It is a progressive disease that develops slowly and typically becomes apparent after 40 or 50 years of age.
The most common symptom of COPD is shortness of breath or a constant need for air. Other common symptoms include a chronic or consistent cough, sputum (mucous production), and reduced energy or increased fatigue. Other common symptoms include:
- Frequent respiratory infection
- The blueness of lips, fingernail beds
- Wheezing
For many patients with COPD, daily activities, such as walking up a short flight of stairs or carrying a suitcase, and even daily routine activities can become difficult as the condition gradually worsens. With each progression or stage of COPD, the patient may also experience exacerbations or what’s commonly known as a COPD flair-up. These episodes can be seriously disabling and result in the need for urgent medical care (including hospitalization) and sometimes death.
How is COPD diagnosed? #
Arguably the most difficult problem associated with COPD is a correct diagnosis.
Chronic obstructive pulmonary disease is usually suspected in people who experience the symptoms described above. However, many patients – especially those who are older or obese believe that this condition is due to ‘old age’ or simply being out of shape.
As such, several people may be living with onset or early-stage COPD – but simply are not showing serious indicators that stimulate their primary care physician to order a lung function test.
This is the first step in diagnosing COPD or any progressive lung disease. The main test completed is known as spirometry – which measures how much and how quickly a person can forcibly exhale air. Depending on the results of this test, the patient’s demographic data, and exposure to risk factors, the doctors will determine if additional testing is required.
The second step is an escalation of lung function testing – which measures the total lung volume. This is often completed by PFT or pulmonary function testing equipment. It’s intended to discover the patient’s ability to inhale, exhale, and most importantly, how blood gases are diffused within the body.
The secondary tests are often completed by a lung health specialist or pulmonologist or cardiovascular professional – as there is a growing link between progressive lung disease and cardiovascular disease.
Other tests for diagnosing COPD #
- Lung (pulmonary) function tests. Other tests include measurement of lung volumes and diffusing capacity, a six-minute walk test, and pulse oximetry
- Chest x-ray
- CT scan
- Arterial blood gas analysis
- Laboratory tests – to determine if the patient suffers from an alpha-1-antitrypsin deficiency
Once the type of obstruction and total lung volume has been assessed, CT scans and imagery can confirm the progression and precise source of the obstruction. These factors, along with multiple blood tests and analysis will determine which disease the patient suffers.
How is COPD treated? #
The availability of diagnostic and treatment options for COPD differs across varying resource settings. However, general treatment focuses on three objectives:
Mitigating exposure to COPD contributing factors #
Determine the root source of exposure that led to COPD. For patients who smoke tobacco, providing resources to help them quit smoking is a crucial first step in stopping the progression of the disease.
Respiratory therapy #
A growing treatment with COPD and asthma is completing respiratory therapy – or the process of exercising the lungs. Depending on the progression of the disease, respiratory therapy can range from walking or static bicycle riding, to simply playing the harmonica. Oxygen therapy is another important treatment that helps patients living with COPD.
COPD medication #
There are two types of medication typically used with COPD patients – medication for maintenance and for treating exacerbations.
Daily maintenance therapies for COPD are designed to help patients breathe better throughout the day. Depending on the severity of COPD symptoms, the doctor may prescribe daily maintenance therapy. Common therapies include oral medications, maintenance inhalers, and nebulized solutions.
The second type of medical treatment is to manage exacerbations. This includes the use of bronchodilators, steroids, and antibiotics.
Treatments for COPD are determined based on specific lung diseases. For example, treatments for Chronic Bronchitis are not always beneficial for those living with Emphysema and vice-versa. The progression of the disease, comorbidity factors, and patient discipline are likewise critical factors in the effective treatment of COPD.
The importance of correctly diagnosing COPD #
One of the major concerns for COPD management is its overlap with other diseases, especially asthma. Unlike COPD, which usually has a later onset in patients, asthma typically occurs in childhood. As per the reports of CDC, more than 6 million children and 16.5 million adults in the United States have asthma.3
Correctly diagnosing a patient with COPD or asthma is a crucial first step to quality care, management, and helping them live a higher quality of life. Using accurate lung function testing equipment – from spirometry to PFT devices helps the clinician receive quick and robust results – giving them a better pathway to continue with secondary testing.
ndd Medical Technologies line of EasyOne Air and EasyOne Pro lung function testing solutions are designed for optimal efficiency, with user-friendly features, and can complete tests quicker – without the need for constant calibration.
The EasyOne Air was designed to streamline and improve lung function testing. It is a user-friendly spirometer that can be used in an office or directly onsite. Being a portable spirometer, clinicians have the power and flexibility to test at the point of care making is easier to attend public health fairs or onsite screening events. This broadens the reach of lung function testing and provides a baseline for unsuspecting people to discover the true performance of their respiratory system.
A practical example of this type of screening is the events hosted by the aforementioned Right2Breathe non-profit. They complete more than 500 free spirometry tests at their events using the ndd Medical Technologies EasyOne Air portable, bluetooth-enabled spirometer.
Over a period of six motorsports events from 2016 till 2019, they have discovered that nearly 25% of all those screened have at least a 20% obstruction. The results of their spirometry exam are documented – which gives the patient a scorecard to provide to their primary healthcare provider.
Most of these patients had no idea a problem existed. And since this program started in 2016, several of them have been officially diagnosed and on the pathway to better treatment and management with their specific lung disease.
COPD will continue to pose a threat and remain a significant public health burden for the foreseeable future, globally. With risk factors largely unchanged, demographic developments in high-income countries and a significant increase in non-communicable diseases in low-income countries is expected to accelerate this health risk.
Using accurate, robust, and consistent lung function equipment is the crucial first step for healthcare professionals to diagnose COPD correctly. If you’d like to learn more about ndd Medical Technologies line of lung function testing equipment, view our products below.
Centers for Disease Control and Prevention. National Health Interview Survey. National Center for Health Statistics, 2015 ↩︎